MEDICALLY REVIEWED BY
Dr. Batul Patel (Dermatologist)
Medical Director – The Bombay Skin Clinic
Dr. Batul Patel is an award winning certified dermatologist, honoured as the “Dermatologist of the Year 2023” at the national level by The Economic Times. View profile
What Is PCOS Acne | Why PCOS Causes Acne | Treatment Options | Expected Results | Treatment Cost
PCOS acne can be frustrating because it often feels cyclical. The skin may improve for a while, then flare again around the jawline, chin, lower cheeks, or neck. For many women, it is not just “adult acne”. It can be a skin sign of a broader hormonal pattern.
At Acne Freedom Clinic in Mumbai, we focus on two things together: controlling active breakouts, oiliness, marks, and scar risk, and checking whether a hormonal driver is keeping the acne active.
What is PCOS acne?
How PCOS and acne are linked
PCOS, short for polycystic ovary syndrome, is a common hormonal condition. One of its visible skin signs can be acne, especially when androgen activity is higher and oil production increases. Insulin resistance can also worsen this pathway in some patients. [1,6]
PCOS acne often needs a broader view, including periods, facial hair growth, scalp thinning, weight changes, and other signs of androgen excess. [1,2,6]
Is PCOS acne different from regular acne?
It can look similar, but the pattern is often more persistent and more relapse-prone. PCOS acne commonly shows up as recurring inflammatory lesions, deeper breakouts, increased oiliness, and flares that continue into the 20s, 30s, or later, rather than settling after the teenage years. [2,3]
Not every woman with jawline acne has PCOS, and not every woman with PCOS has severe acne. But when acne is stubborn, cyclical, or paired with other hormonal signs, it is worth assessing beyond skincare alone. [2,6]
What does PCOS acne usually look like?
Common signs, jawline acne, deep breakouts, oiliness, and recurring flares
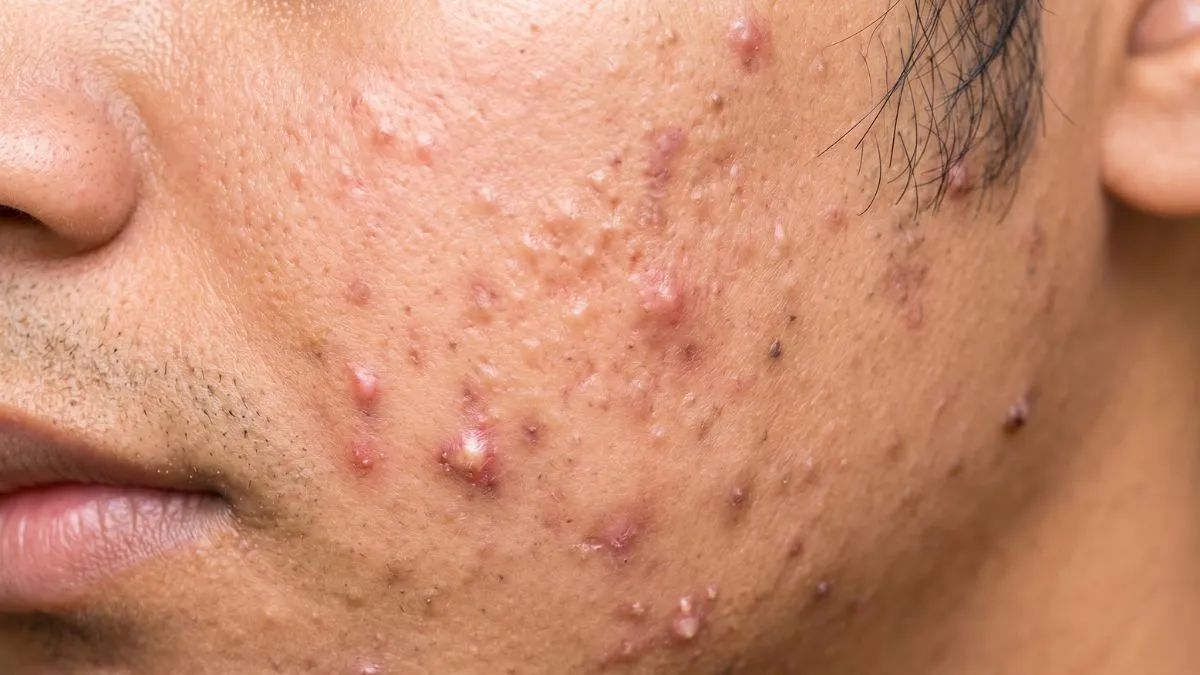
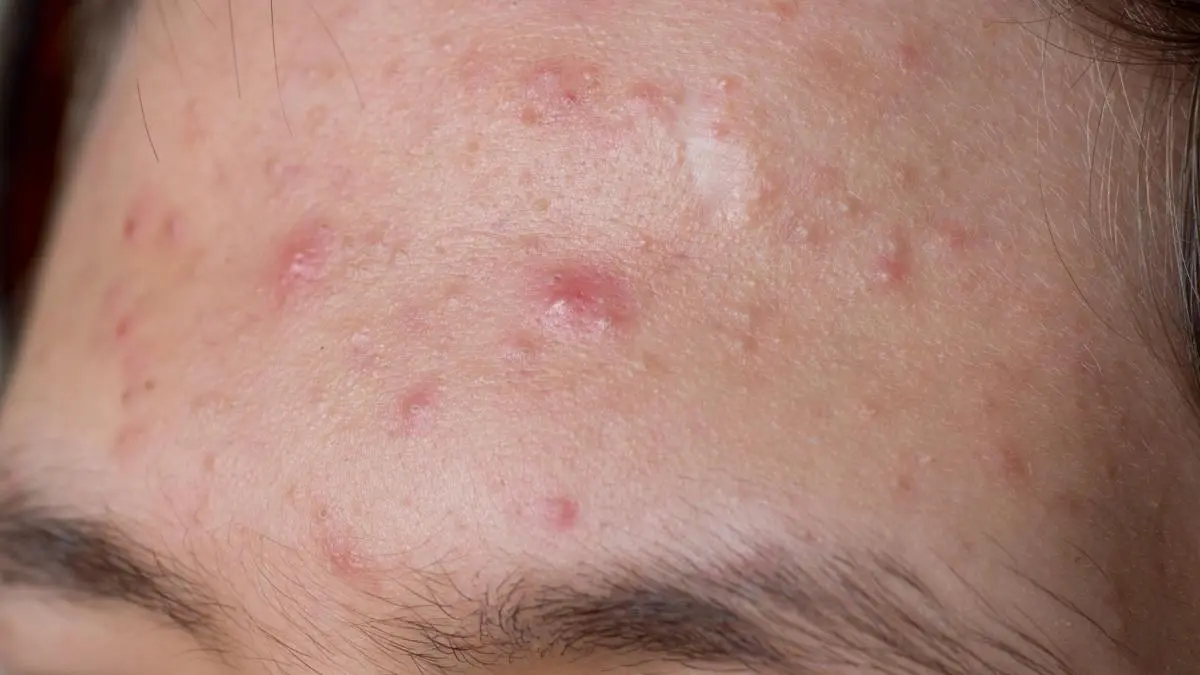
PCOS acne often affects the lower face. Many patients notice painful bumps around the chin, jawline, neck, and lower cheeks. Some also have whiteheads, blackheads, or a generally greasy skin feel by midday.
Another clue is recurrence. The acne may settle, then flare again with stress, poor sleep, irregular cycles, or stopping treatment too soon. In Mumbai, humidity, makeup, and long commuting hours can add to congestion on already acne-prone skin.
When acne may suggest an underlying hormonal issue
Acne deserves a closer hormonal look when it is persistent in adulthood, concentrated on the lower face, associated with irregular periods, excess facial hair, scalp thinning, or when it resists standard treatment. Adult female acne can be a clinical expression of hyperandrogenism, and PCOS is one important possibility. [2,6]
This does not mean every breakout needs a hormone work-up. It means pattern matters. A dermatologist can help decide when the acne is behaving like routine comedonal acne and when it may need wider evaluation.
Why does PCOS cause acne?
The role of androgens, excess oil, clogged pores, and inflammation
Acne develops through a mix of excess oil, clogged follicles, bacterial overgrowth, and inflammation. In PCOS, androgen excess can push oil glands to produce more sebum, which makes pores more likely to clog and inflamed breakouts more likely to form. [2,4]
Creams may help, but if the hormonal trigger remains active, the skin may keep cycling through new lesions. This is why cystic acne treatment often requires a more comprehensive, medically guided approach.
Why PCOS acne can keep coming back if the root trigger is missed
A good acne routine can reduce flare intensity, but recurrence is common when the plan focuses only on the pimple and not on the pattern behind it. This is one reason guidelines encourage proper assessment, maintenance, and specialist review when acne is persistent or when there are signs that suggest a broader endocrine driver. [1,3,4]
The goal is steady control, lower scar risk, and calmer skin over time.
What are the advantages of treating PCOS acne early?
- Early treatment can reduce the risk of acne marks and long-term textural scarring. [3,4]
- It may shorten the cycle of frequent flare-ups and reduce the urge to keep changing products.
- It helps identify when acne may be linked to PCOS or another hormonal issue, so care is not delayed. [1,2,6]
- It allows a safer plan for Indian skin tones that are more prone to post-inflammatory pigmentation after repeated inflammation or picking.
- It can improve daily comfort, confidence, and consistency with skincare.
Who may be a good candidate for PCOS acne treatment?
You may be eligible if
- You have ongoing acne in adulthood, especially around the chin, jawline, lower cheeks, or neck.
- Your skin is oily, breakout-prone, and leaves marks easily after inflammation.
- You have acne that seems cyclical, stubborn, or only partially responsive to over-the-counter routines.
- You are willing to follow a structured plan and review it over time rather than expecting overnight change.
- You want a dermatologist-led assessment before acne leaves more marks or scars.
You may need extra caution or a different plan if
- You are pregnant, breastfeeding, or trying to conceive, because some acne options may not be suitable then. [3,4]
- You have very sensitive skin, active dermatitis, frequent barrier damage, or a history of strong reactions to peels or actives.
- You are dealing with rapid worsening, severe nodules, or scarring, which may need earlier specialist escalation. [3,4]
- You have irregular periods, significant facial hair growth, scalp thinning, or weight changes, where a parallel gynaecology or endocrine review may be useful. [1,2,6]
- You are mainly concerned about acne scars rather than active acne, because the treatment priorities are different.
How do we assess PCOS acne at Acne Freedom Clinic?
Skin assessment, acne pattern review, and trigger mapping
The first step is understanding what is active right now. We assess whether you mainly have clogged pores, inflamed acne, deep painful lesions, acne marks, early scarring, or a mix of all five. We also review where the acne sits, how long it has been happening, what seems to trigger it, and what your skin has already tried.
PCOS acne is not managed well by a one-size-fits-all routine. One patient may need a barrier-friendly reset first. Another may need acne control plus mark management. Another may need scar prevention because the lesions are deep and recurrent.
When we may advise a gynaecology or endocrinology review as part of the plan
If the skin story suggests a hormonal driver, we may advise a parallel review with a gynaecologist or endocrinologist. That can be especially useful if acne is paired with irregular periods, unwanted facial hair, scalp thinning, fertility concerns, or metabolic signs such as weight gain around the waist or darkening in body folds. [1,6]
This does not replace dermatologist care. It supports it.
How does PCOS acne treatment work?
Daily skincare and prescription support for hormonal acne
PCOS acne treatment usually starts with calming the acne cycle, not over-treating the skin. The core plan often includes a gentle cleanser, a light non-comedogenic moisturiser, sun protection that suits acne-prone skin, and dermatologist-guided medical treatment based on acne type and severity. Maintenance matters because acne often relapses when treatment is stopped too early. [3,4]
We also look at everyday triggers such as picking, harsh scrubs, too many products, hair oils touching the face, occlusive makeup, and routines that damage the skin barrier.
In-clinic supportive options for active acne, congestion, and post-acne marks
When suitable, in-clinic procedures can support the medical plan. At Acne Freedom Clinic, supportive options may include acne-focused peels such as the Acne Erase Peel, medi-facial style congestion control such as the Acne Healing Facial, and selected clinic protocols within the Acne Freedom Program when the skin needs a broader combination approach.
For some patients, selected light-based or laser-based treatments may be considered as adjuncts for active acne or post-acne marks. These are not first-line answers for every case, and evidence across light-based acne treatments is mixed, so selection needs to be careful and personalised. [3,5]
How combination plans are personalised for Mumbai weather, lifestyle, and skin tone concerns
In Mumbai, acne care needs to work in real life. Heat, humidity, sunscreen fatigue, makeup for work, long office hours, travel, and social schedules all influence what a patient can actually follow. A routine that looks ideal on paper but feels greasy or irritating in this climate often fails.
We also plan with Indian skin tones in mind. Repeated inflammation and aggressive procedures can leave brown marks more easily, so the aim is steady improvement rather than over-correcting the skin.
What results can you realistically expect, and how long does it take?
Early changes in oiliness and inflamed breakouts
The first wins are usually better control, not instant perfection. Many patients first notice that the skin feels less greasy, the deepest inflamed lesions settle faster, and the frequency of fresh painful breakouts starts to reduce. Guideline-based acne care is usually assessed over weeks, not days. [3,4]
PCOS acne often improves in layers. Active inflammation may settle before marks do. Texture takes longer than redness. And maintenance is usually part of the plan, especially if hormonal drivers remain active.
When acne marks and texture may start improving
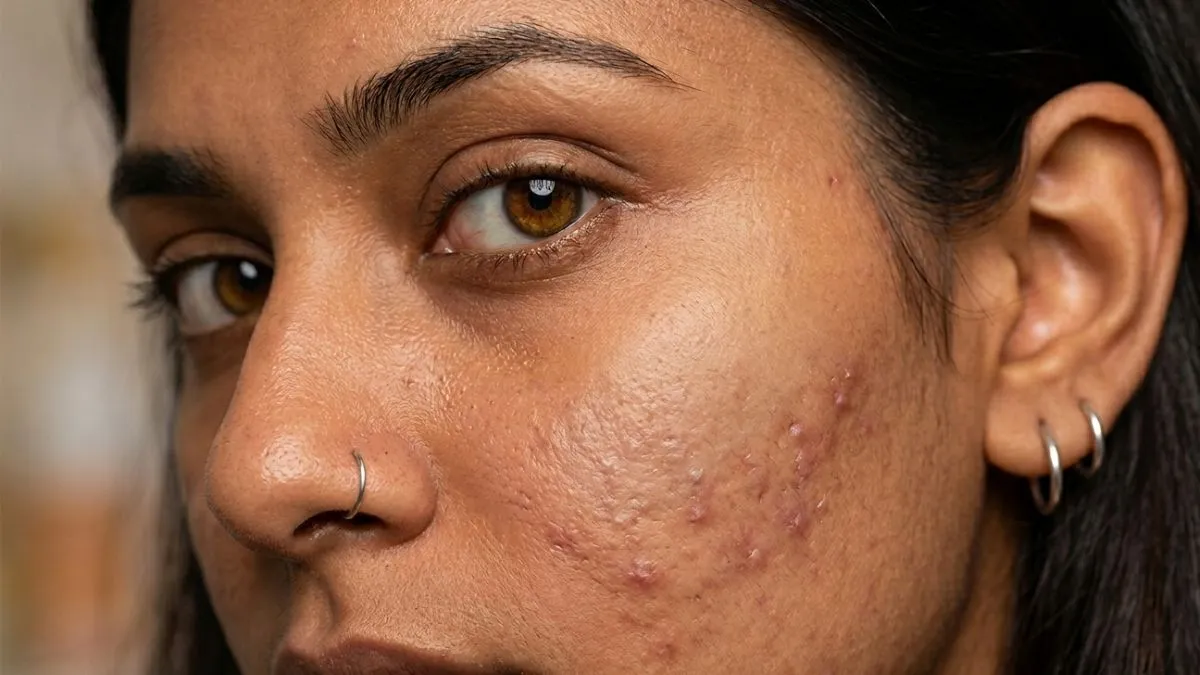
Post-acne marks often fade more slowly than the acne itself, especially in Indian skin. Brown marks can linger after inflammation, and early textural change can take longer still. This is where a mix of acne control, sun protection, and selected in-clinic support can be useful.
If there is established scarring, that becomes a separate treatment conversation. Active acne should usually be stabilised first so that scar treatment is not trying to catch up with ongoing inflammation.
Why maintenance matters in PCOS-related acne
One of the most important mindset shifts in PCOS acne is understanding maintenance. Acne that is hormonally influenced often behaves like a chronic tendency, not a short infection that disappears after a brief course. NICE and AAD-based care both stress maintenance and follow-up because relapse is common if the underlying pattern is not kept under control. [3,4]
That does not mean you stay on the same plan forever. It means the plan is stepped down thoughtfully rather than stopped suddenly.
Which is better for PCOS acne, skincare, medicines, peels, or laser-based treatments?
When medical acne treatment matters more than procedures
When acne is active and hormonal, the medical plan usually matters more than any single procedure. That is because the skin needs fewer new lesions first. If breakouts keep forming, procedures alone often give only partial or temporary improvement. [2,3,4]
When dermatologist-led procedures can be a supportive option
Procedures can still be useful. They may help with congestion, oiliness, superficial marks, and recovery support in selected cases. At our clinic, they are best viewed as supportive tools inside a bigger acne plan, not as a stand-alone fix for the hormonal condition itself.
Light-based treatments need especially careful counselling. Some patients do benefit, but overall evidence is mixed and device-specific, so treatment choice should be conservative and dermatologist-led. [5]
PCOS acne vs regular adult acne, why the plan may differ
Regular adult acne may be driven more by cosmetics, stress, barrier damage, genetics, or milder hormonal shifts. PCOS acne is more likely to involve a stronger androgen pattern, more relapse, and a need for parallel medical evaluation. [1,2]
What is the cost of PCOS acne treatment at the Acne Freedom Clinic?
The cost depends on what your skin actually needs. Factors usually include the severity of active acne, whether marks or scars are already present, whether the plan is skincare-led or includes clinic procedures, the type of procedure chosen, how many sessions are advised, and how reactive or pigmentation-prone your skin is.
A personalised assessment is the safest way to estimate cost because it avoids under-treating severe acne and avoids over-treating mild acne. It also helps separate what is necessary now from what can wait until the skin has stabilised.
FAQs
Is jawline acne always due to PCOS?
No. Jawline acne can happen without PCOS. Cosmetics, stress, genetics, occlusion, and routine mistakes can all contribute. But if jawline acne is persistent or comes with irregular periods, unwanted facial hair, or scalp thinning, PCOS should be considered. [2,6]
Can I have PCOS if acne is my main symptom?
Yes, it is possible. Acne can be one of the visible signs of androgen excess. But acne alone does not confirm PCOS, which is why diagnosis should not be self-made from skin changes only. [1,2,6]
Can chemical peels or facials cure PCOS acne?
No. Peels and facials do not treat the hormonal condition itself. They may support acne control, reduce congestion, and help with marks in selected patients, but they work best as adjuncts within a broader plan. [3,5]
How long does PCOS acne treatment usually take to show visible improvement?
It varies, but most patients should think in weeks to months, not days. Early reduction in active inflammation may come before marks improve, and maintenance is often part of long-term control. [3,4]
What if I also have acne marks or acne scars?
That is common. We usually prioritise control of active acne first, then add mark or scar-focused treatment in a staged way. This helps reduce new lesion formation while we work on older damage.
Which doctor should I see for PCOS acne in Mumbai?
Start with a dermatologist if acne is the main concern. If the skin pattern suggests a hormonal issue, a gynaecologist or endocrinologist may be added to the plan. In many patients, the best results come from coordinated care rather than choosing only one specialty. [1,2,6]
Sources
- Teede HJ, Tay CT, Laven J, et al. Recommendations from the 2023 International Evidence-Based Guideline for the Assessment and Management of Polycystic Ovary Syndrome. Eur J Endocrinol. Link
- Carmina E, Azziz R, Bergfeld W, et al. Female Adult Acne and Androgen Excess: A Report From the Multidisciplinary Androgen Excess and PCOS Committee. J Endocr Soc. Link
- National Institute for Health and Care Excellence. Acne vulgaris: management. NICE guideline NG198. Link
- Reynolds RV, Yeung H, Cheng CE, et al. Guidelines of care for the management of acne vulgaris. J Am Acad Dermatol. Link
- Barbaric J, Abbott R, Posadzki P, et al. Light therapies for acne: abridged Cochrane systematic review including GRADE assessments. Br J Dermatol. Link
- Endocrine Society. Polycystic Ovary Syndrome. Endocrine.org. Link

MEDICALLY REVIEWED BY
Dr. Batul Patel (Dermatologist)
Medical Director – The Bombay Skin Clinic
Dr. Batul Patel is an award winning certified dermatologist, honoured as the “Dermatologist of the Year 2023” at the national level by The Economic Times. View profile